|
|
|
|
|
|
|
|
Bobby Smyth,J Barry,E Keenan,K Ducray
|
|
|
|
Ir Med J. 2010 Jun;103(6):176-9.
|
|
BP Smyth1,2, J Barry2, E Keenan1, K Ducray3
1Addiction Service, Bridge House, Cherry Orchard Hospital, Ballyfermot, Dublin 10
2Department of Public Health & Primary Care, Trinity College, Dublin 2
3Drug Treatment Centre Board, 30/31 Pearse St, Dublin 2
Abstract
We conducted a prospective follow-up study of consecutive opiate dependent patients admitted to a residential addiction treatment service for detoxification. We measured the rate of relapse following discharge, and sought to identify factors that were associated with early relapse (i.e. a return to daily opiate use). Follow-up interviews were conducted with 109 patients, of whom, 99 (91%) reported a relapse. The initial relapse occurred within one week in 64 (59%) cases. Multivariate survival analysis revealed that earlier relapse was significantly predicted by younger age, greater heroin use prior to treatment, history of injecting, and a failure to enter aftercare. Unexpectedly, those who were in a relationship with an opiate user had significantly delayed relapse. Those who completed the entire six-week inpatient treatment programme also had a significantly delayed relapse. In order to reduce relapse and the associated increased risk of fatal overdose, services providing residential opiate detoxification should prepare people for admission, strive to retain them in treatment for the full admission period and actively support their entry into planned aftercare in order to improve outcome.
Introduction
It has been known for many years that addictive disorders tend to run a chronic relapsing course1. Despite the robust evidence demonstrating the effectiveness of methadone maintenance in the treatment of opiate dependence, many patients seek abstinence based treatments. A growing body of experts, both nationally and internationally, are calling for much greater provision of such treatments2,3. International studies have found that the majority of patients lapse within one month of discharge4-6. Heavier heroin use prior to treatment, greater criminal justice problems, failure to complete treatment and fewer coping mechanisms were all identified as factors which may predict early relapse5. Relapse following detoxification based treatments carries a substantial mortality risk due to accidental overdose, especially for heroin injectors7,8. We decided therefore to measure the rates of lapse and relapse in a group of opiate dependent patients undergoing inpatient detoxification in Dublin, and to identify patient and treatment adherence characteristics associated with early relapse in order to better identify those patient groups who are most suitable for such treatment.
Methods
The addiction treatment services available in the Dublin area underwent a vast expansion between 1992 and 1997. Around this time it was estimated that there were approximately 13000 heroin users in Dublin9. Cuan Dara was opened in Dublin in 1995. It was a specialist inpatient Drug Dependency Unit, dealing primarily with opiate dependence. A psychiatrist assessed patients prior to admission to diagnose dependency and to determine their suitability to undergo detoxification. The inpatient abstinence orientated treatment programme lasts six weeks. Opiate detoxification using methadone occurred during the first ten days followed by lofexidine for seven days10. Psychosocial interventions included group therapy, individual therapy and in addition family therapy was provided where needed. All patients were expected to participate in these treatments. During admission patients were encouraged to access aftercare following discharge. Cuan Dara offered a structured aftercare programme where patients could return for group counselling once per week and further support. Alternatively, they could attend their counsellor at their local addiction treatment services for aftercare, this counsellor usually playing a central role in the initial referral of the patient for residential treatment.
The study population comprised consecutive patients admitted to the abstinence orientated treatment programme in Cuan Dara with a diagnosis of opiate dependence, between June 1995, and December 1996 from the greater Dublin area. All participants gave informed consent and took part in the study voluntarily. Pre-treatment characteristics were obtained from the semi-structured assessment interview completed by patients upon admission to Cuan Dara. Follow up interviews occurred between June 1998 and March 1999. These were carried out by eight outreach workers who administered a structured questionnaire directly to the participants. Lapse was defined as any misuse of an opiate following discharge from treatment. Relapse was defined as a return to a pattern of daily opiate use. Patients provided information on lapse, relapse and timing of same at the follow-up interview. In order to identify variables, which were associated with early relapse, we undertook a Kaplan-Meier survival analysis. The log rank statistic was used as the measure of statistical significance. We then completed a multivariate analysis using Cox regression analysis in order to identify those variables which were independently associated with relapse. Variables were selected for entry into the final regression equation using the forward and backward selection technique.
Results
Of the 160 patients who were admitted to Cuan Dara during the study period, 149 were eligible to participate in the study, the remaining eleven being admitted to stabilise on methadone. Of the 149 patients, five patients died during the follow-up period and thirty-five could not be traced. We interviewed 109 (76%) of those who were still alive. We examined the baseline socio-demographic, drug misuse and treatment adherence characteristics of all patients and found no significant differences between those interviewed and those not interviewed. Of the 109 interviewees, 89% were unemployed, 36% were female and their median age on admission was 22 years (range 16-37 years). Heroin was the main opiate of misuse for 96 (88%) patients, with the median duration of opiate use prior to admission being four years (range 1-18 years). The median duration of inpatient treatment was 24 days with eighty-six (79%) patients completing the methadone detoxification phase of in-patient treatment, but only 42 (39%) completing the full six-week treatment programme. Forty-three (39%) entered aftercare following discharge. The median period from discharge to interview was 29 months (range 18-42 months).
Following discharge 103 (94%) of the 109 patients interviewed reported a lapse, and 99 (91%) reported a
relapse. Within one week of discharge, 72 (66%) had lapsed and 64 (59%) had relapsed (see Figure 1). Within one month these proportions had risen to 80% and 71% respectively. Relapse occurred within a week of the initial lapse in 74% cases. The gap between lapse and relapse was greater than one month in only 15% of cases. Eighty percent of those who relapsed did so within the first month after discharge. When analysing pre-treatment characteristics on univariate analysis, earlier relapse was found to be significantly associated with a history of injecting, previous detoxification treatments and a history of imprisonment. Early relapse was also predicted by failure to complete the methadone detoxification component of in-patient treatment, by failure to complete the full inpatient treatment programme and by a failure to enter aftercare. The relationship between program completion and relapse is demonstrated in Figure 1.
Figure 1: Avoiding relapse during the first six months following inpatient opiate detoxification: Influence of planned discharge
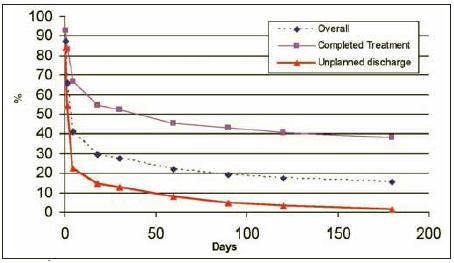
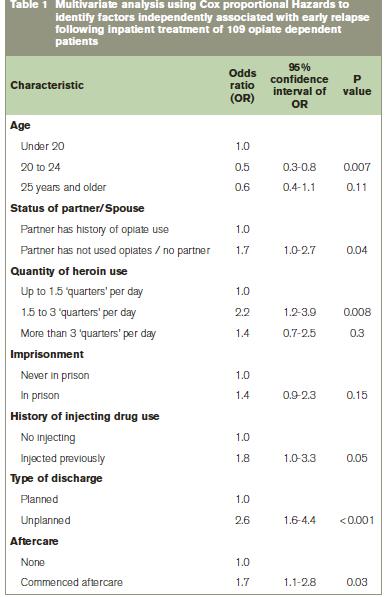
When multivariate analysis was performed on the data it emerged that younger age, a history of injecting, greater heroin use, not being in a relationship with an opiate using partner, failure to complete the treatment programme and failure to enter aftercare were each significantly associated with earlier relapse (See Table 1). Ninety two percent of relapsers re-entered treatment prior to follow-up interview, with the median gap from relapse to re-entry being four months. Most (71%) of these accessed methadone maintenance treatment in the first instance. However, of those who relapsed, 54% did undertake at least one further detox during the follow-up period.
Discussion
From these results it can be seen that following inpatient opiate detoxification, lapse and relapse are common and that lapse was quickly followed by relapse in the majority of cases. Our figures of a one-month lapse rate of 80% are very similar to those found in some previous studies of opiate users6,11. Relapse is common to all addictions and the relapse rates detected here for opiate dependent subjects have much in common with those found for other addictive disorders12. The findings support Rounsaville’s assertion that relapse and relapse prevention represent the major challenges faced by both clinicians and researchers who work with substance abusers1. We found that two-thirds of this young population of opiate dependent patients lapsed, and three-fifths had relapsed, within a week of discharge. As in the study performed by Gossop et al, this supports the view that there is a “critical period” very shortly after discharge when patients are particularly susceptible to using opiates4. This indicates the importance therefore of pre-discharge planning and prompt introduction of aftercare support during this high-risk period13.
In our study, on univariate analysis, it emerged that injectors and those who had been in prison demonstrated significantly earlier relapse. In contrast to these characteristics, which are linked to more chronic opiate misuse and similar to findings by Gossop et al5, younger age was also associated with earlier relapse in this study. Youth has previously been cited by others as a negative predictor of treatment outcome14. While it would be unreasonable to deny patients with these characteristics access to this treatment option, they should be borne in mind by patients and treatment providers when weighing up the potential risks and benefits of detoxification. As in previous studies we also found that patients who persisted with the complete six week inpatient treatment program and those who accessed aftercare experienced statistically and clinically significant reductions in relapse15,16. Centres providing residential addiction treatment must strive to maximise both treatment completion rates and successful progressions into aftercare. Exploration of aftercare treatment options should occur before admission8. There are an increased range of residential and daycare aftercare options now available in Ireland. An evaluation of one of the residential aftercare options has yielded encouraging outcomes, with 60% of those who accessed treatment being abstinent from all drugs at one year follow-up17. NTORS found that patients who regularly attend 12-step groups after residential treatment are more likely to sustain abstinence from alcohol and opiates16.
Treatment re-entry rates were very satisfactory with 92% of relapsers re-accessing treatment, and the median gap from relapse to re-entry was four months. These figures are encouraging and may reflect the fact that once patients are linked in with services, they find re-entry into treatment easily attainable through aftercare programmes, and addiction counselling. Many did ultimately attain their initial goal of abstinence10. The five deaths that occurred highlight the risks associated with this disorder and the potential hazards of pursuing abstinence. It is this risk of death; especially in the first month after completion of detoxification, that sets opiate addiction apart from other addictive disorders7. Patients accessing this treatment option must be made fully aware of the risks of overdose prior to treatment entry. There are potential medical strategies to reduce both relapse and overdose risk, the most promising of which is naltrexone, a treatment that is still probably underutilised in Ireland to date18.
We acknowledge that one limitation of the study relates to the length of time between patient discharge and interview. This may contribute to retrospective recall bias by patients. If recall bias were present it would have reduced our ability to detect significant associations between relapse and the factors which predict it. However we did find many significant associations with relapse and the results have face validity when compared to the findings of other relapse studies. The fact that relapses typically occurred so close to discharge in most instances is likely to have assisted patients in accurate recall. Previous studies report that drug users are able to give valid self-reports about their drug use in settings where social desirability does not play an important role19. A second limitation relates to the fact that relapse is increasingly recognised as a complex product of a dynamic interaction of many more distal, intermediate, proximal and transitional factors than those relatively few factors considered by this study20.
As Ireland launches a new National Drugs Strategy for 2009-16, we believe that the findings from this study, albeit conducted in the late 1990s, are very relevant. The patient population and approaches to residential detoxification remain largely the same. There is a growing political and professional pressure to move away from methadone maintenance and to increase abstinence based treatment options3. The international literature has provided some guidance on strategies which could improve the outcomes achieved in this patient group8. Prior to admission, patients should be supported to commence making the psychological and social changes which will facilitate their progression into a drug free lifestyle following completion of residential treatment21. Improved psychological supports, with a specific focus on relapse prevention, during the critical period immediately following discharge from in-patient treatment, and focused efforts to facilitate treatment completion with prompt entry into aftercare, may all contribute to improving patient outcome4,8.
Correspondence: BP Smyth
Addiction Service, Bridge House, Cherry Orchard Hospital, Ballyfermot, Dublin 10
Email: [email protected]
References
1. Rounsaville BJ. Clinical Implications of relapse research. In F. M. Tims & C. G. Leukefeld (Eds.), Relapse and recovery in drug abuse; 172- 184. Rockville, MD: National Institute on Drug Abuse, 1986
2. McKeganey NP. The challenge to UK drug policy. Drugs: Educ Prev and Policy 2007; 14: 559-571
3. Corrigan D, O'Gorman A. Report of the HSE Working Group on Residential Treatment & Rehabilitation (Substance Users). Dublin: Health Service Executive, 2008
4. Gossop M, Green L, Phillips G, Bradley B. Lapse, Relapse and Survival among Opiate Addicts after Treatment. A Prospective Follow-up Study. B J Psych, 1989; 154: 348-353.
5. Gossop M, Stewart D, Browne N, Marsden J. Factors associated with abstinence, lapse or relapse to heroin use after residential treatment: protective effect of coping responses. Addiction 2002; 97:1259-1267.
6. Broers B, Giner F, Dumont P, Mino A. In-patient opiate detoxification in Geneva: follow-up at 1 and 6 months. Drug Alc Depend 2000; 58:85-92.
7. Strang J, McCambridge J, Best D, Beswick T, Bearn J, Rees S, Gossop M. Loss of tolerance and overdose mortality after inpatient opiate detoxification: follow up study. BMJ 2003; 326,: 959-960.
8. NICE. Drug Misuse. Opioid detoxification. London: National Institute for Health & Clinical Excellence, 2007
9. Comiskey CM, Barry JA. Capture-Recapture study of the prevalence and implications of opiate use in Dublin. Eur J Pub Health 2001; 11:198-200.
10. Smyth BP, Barry J, Lane A, Cotter M, O'Neill M, Quinn C, Keenan E. Inpatient treatment of opiate dependence: Medium term follow-up outcomes. B J Psych 2005; 187, 360-365
11. Chutuape MA, Jasinski DR, Fingerhood M I, Stitzer ML. One-, Three-, and Six-Month Outcomes after brief Inpatient Opioid Detoxification. Am J Drug Alc Abuse 2001; 27:19-44.
12. Hughes J, Keely J, Naud S. Shape of the relapse curve and long-term abstinence among untreated smokers. Addiction 2004; 99:29-38.
13. Chutuape MA, Silverman K, Stitzer M. Contingent reinforcement sustains post-detoxification abstinence from multiple drugs: A preliminary study with methadone patients. Drug Alc Depend 1999; 54: 69-81.
14. Center for Substance Abuse Treatment. Patient matching: Historical perspective and overview. In Matching treatment to patient needs in opioid substitution therapy: Treatment improvement protocol (TIP) 20 (DHHS Publication No. SMA 95-3049). Rockville, MD: U.S. Department of Health and Human Services, Substance Abuse and Mental Health Services Administration, 2004.
15. Ghosde AH, Reynolds M, Baldacchino AM, Dunmore E, Byrne S, Oyefeso A, Clancy C, Crawford V. Treating an opiate-dependent inpatient population: A one-year follow-up study of treatment completers and noncompleters. Addict Behav 2002; 27:765-778.
16. Gossop M, Stewart D, Marsden J. Attendance at Narcotics Anonymous and Alcoholics Anonymous meetings, frequency of attendance and substance use outcomes after residential treatment for drug dependence: A 5-year follow-up study. Addiction 2008; 103: 119-125.
17. Sweeney B, Browne C, McKiernan B, White E. Keltoi Client Evaluation Study. Dublin: Health Service Executive, 2007.
18. Kunøe N, Lobmaier P, Vederhus JK, Hjerkinn B, Hegstad S, Gossop M, Kristensen Ø, Waal H. Naltrexone implants after in-patient treatment for opioid dependence: randomised controlled trial. B J Psych 2009: 194: 541-546.
19. Langendam M, Haastrecht H, Ameijden J. The validity of drug users’ self-reports in a non-treatment setting: prevalence and predictors of incorrect reporting methadone treatment modalities. Int J Epid 1999; 28:514-520.
20. Donovan DM. Assessment of Addictive Behaviors for Relapse Prevention. In: Donovan DM, Marlatt GA. (Eds.), Assessment of Addictive Behaviors, Second Edition (1- 48). London: The Guilford Press, 2005.
21. Department of Health (England) and the devolved administrations. Drug misuse and dependence: UK guidelines on clinical management. London: Department of Health (England), the Scottish Government, Welsh Assembly Government and Northern Ireland Executive, 2007.
|
|
|
|
Author's Correspondence
|
|
No Author Comments
|
|
|
Acknowledgement
|
|
No Acknowledgement
|
|
|
Other References
|
|
No Other References
|
|
|
|
|