Introduction
A cardiac arrest is a sentinel event in healthcare. Cardiopulmonary resuscitation1, since the late-1950s2, has been a standard of care for these patients. However, the success rate of this treatment protocol remains dismal, and the progress stagnant3. Focus on improving cardiac arrest outcomes through an auditing culture has resulted in the development of the Utstein template4 for cardiac arrest. This template has provided a scaffold for the United States’ collaborative cardiac arrest registry, known as Get With the Guidelines Registry (GWTG-R)5; as well as the more recently developed National Cardiac Arrest Audit (NCAA) initiative among hospitals in the UK and Ireland 6. Factors surrounding in-hospital cardiac arrest incidence and outcome can highlight general aspects of hospital vigilance, system responsiveness and efficacy. This study describes the incidence and outcomes of in-hospital cardiac arrest at Cork University Hospital, for a one year time period (2011). This establishes a baseline prior to the implementation of national early warning scoring (NEWS) systems, designed to improve clinical vigilance for the deteriorating patient.
Methods
Cork University Hospital (CUH) provides tertiary services to a population of over 1.2 million people. In 2011, the number of acute in-patient beds was 518; 44 029 in-patients were treated (with 43 217 coded admissions), and there were 584 in-patient deaths. Our collection of patient information from hospital and general practice records was approved by the Clinical Research Ethics Committee (CREC). Our definition of “In-hospital Cardiac Arrest (IHCA)” is restricted only to patients who occupied a hospital bed in CUH at time of cardiac arrest, who were at least 18 years old; who did not have a do not attempt resuscitation (DNAR) order documented. All adult hospital areas were included in this study. A “cardiac arrest”, per the Utstein-style definition 4 is ‘the cessation of cardiac mechanical activity [which is] confirmed by the absence of a detectable pulse, unresponsiveness and apnoea (or agonal respirations)’. A “return of spontaneous circulation (ROSC)”, refers to patients in whom a pulse was returned, which resulted in a successful completion of CPR. This definition excluded situations with brief returns of pulse during on-going CPR. We calculated cardiac arrest incidence by dividing the number of patients with IHCA, by the number of patients admitted to the hospital that year, (per 1000 admissions). In patients who experienced multiple arrests, the IHCA number includes only the index arrest.
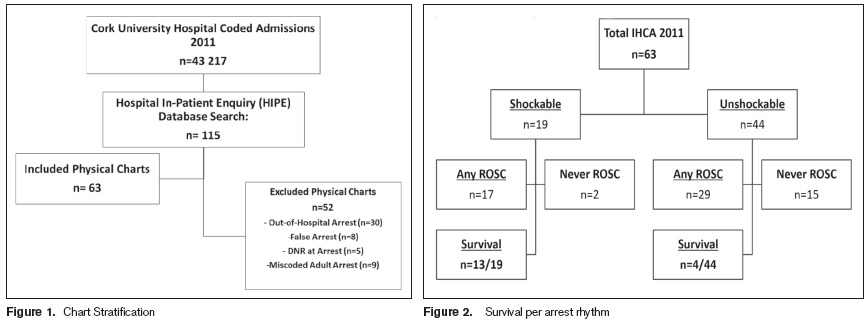
“Resuscitation” was defined as the use of chest compressions and rescue breathing. “Advanced life support”7 measures include invasive airway management, chest compression, drugs administration or defibrillation, with an automated external defibrillator (AED). An “in-hours arrest” refers to an IHCA that occurs Monday to Friday between 09:00 and 16:59; an “out-of-hours” arrest refers to an IHCA that occurs Monday to Friday between 17:00 and 08:59, or any time on a Saturday or Sunday. A “survivor” is any IHCA patient who survived to hospital discharge, after cardiac arrest. “Survival rate” was determined by dividing the number of survivors, by the total IHCA number. “Neurological outcome” was established by calculating the Cerebral Performance Category (CPC) Score7 of that patient at discharge, 6, and 12 months. A “shockable” rhythm refers to ventricular fibrillation, or pulseless ventricular tachycardia (VF or VT); and an “unshockable” rhythm refers to both pulseless electrical activity and asystole. The Hospital In-Patient Enquiry (HIPE) Reporting Database was used to identify eligible patients. Adult (>/= 18 years) in patient cardiac arrest events which occurred from January 1st 2011 through the 31st of December 2011 were included. Figure 1 illustrates chart inclusion criteria.
Cork University Hospital operates to ACLS (advanced cardiac life support) Guidelines8. Physicians are expected to maintain up to date ACLS certification, likewise are Emergency, Intensive Care and Cardiac Care nurses. AEDs can be found on all general wards, as well as in the emergency department (ED), intensive care unit (ICU), cardiac care unit (CCU) and cardiac catheterisation laboratory (cath lab), with all staff trained in their use, irrespective of life support qualification level. Resuscitation equipment is standardised and located on every ward or unit; and within that area, is positioned nearest the highest dependency beds of that area. Cardiac arrest variables which were retrievable and obtained from patient chart included: age; sex; arrest location, time of day, day and month; if the cardiac arrest was witnessed and/or monitored; length of arrest episode; initial rhythm, length of stay prior to event; do-not allow resuscitation (DNAR) status of the patients, rate of ROSC; and likely aetiology. In cases where length of resuscitation was not explicitly charted, data could often be extrapolated via number of CPR rounds (assumed to have two minute intervals).
Outcome data included survival rate, neurological disposition (CPC score) and functional independence of survivors (activities of daily living independence). Outcome data was obtained through the patient’s hospital notes, or via telephone contact with the patient’s General Practitioner. All data was manually entered into a computer database (Microsoft Excel 2003, Microsoft Corporation, Mountain View, CA USA). All statistical analyses were conducted using R Version 2.6.0 (Free Software Foundation, Boston, MA). Descriptive statistics were used to describe data. Logistic regression was used to analyse ROSC and survival associations, as well as complex abnormally distributed variables.
Results
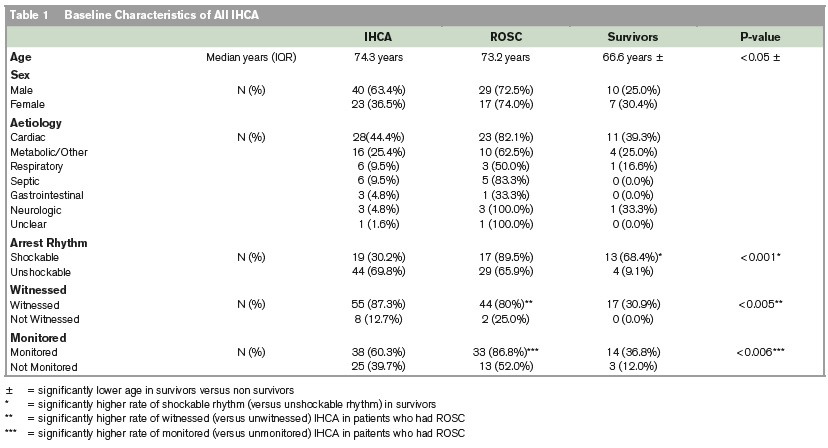
HIPE identified 115 coded in-hospital cardiac arrest cases. These charts were retrieved and reviewed (Figure 1). There were 63 cases which met IHCA criteria. There were n=46/63 (73.0%) patients who achieved ROSC, n=21/63 (33.3%) who achieved a ROSC of greater than 20 minutes, and n=17/63 (27.0%) survived to be discharged from hospital alive (Table 1).
Location
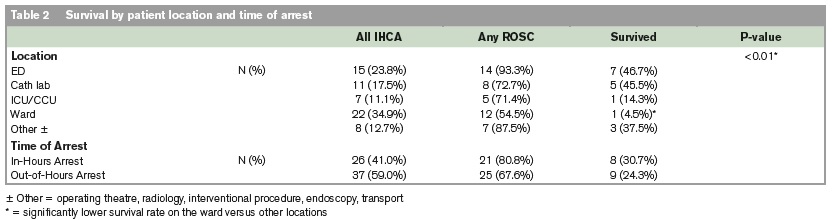
Cardiac arrest outcomes differed on the hospital wards compared to other areas of the hospital, with ROSC rates of 12/22 (54.5%) versus 34/41 (82.9%), p=0.03; and survival rates 1/22 (4.5%) versus 16/41 (39.0%), p=0.01, respectively, (see also Table 2). Compared to a witnessing rate of n=55/63 (87.3%) among all IHCA, only n=44/63 (71.4%) of the ward-based cardiac arrests were witnessed. Within the emergency department (ED), n=6/15 (40.0%) cardiac arrests had a primarily cardiac aetiology, whereas only n=3/22 (13.6%) of those which took place on the ward had a primarily cardiac aetiology.
Length of Stay Prior to Arrest
There were n=24/63 (38.1%) of IHCA patients who had their cardiac arrest on day-one of admission, with, n=11/24 (45.8%), survivors, in that category. Of those IHCA patients who had their cardiac arrest after day-one of their admission, n=6/39 (15.4%) survived. There were two cardiac arrests (n=2/15, 13.3%) that occurred in the ED > 24 hours after registration while the patients were boarded awaiting an inpatient bed. Only (n=1/22, 4.5%) of ward-based cardiac arrests happened on day-one of admission. Of all IHCA patients who had a cardiac arrest on day-one of admission, n=13/24 (54.1%) were shockable. IHCA patients who had a cardiac arrest after day-one of admission, were only shockable in n=6/39 (15.4%) of cases. Length of stay prior to arrest was significantly different between a shockable and unshockable rhythm (p=0.002), and also between survivors and non-survivors, by logistic regression (p=0.01). The single ward survivor arrested on day 22 of admission. Median days of stay prior to arrest were significantly different between shockable (0 days) and unshockable rhythm (4.5 days), p-value < 0.002; and also between survivors (0 days) and non-survivors, (4.0 days), p-value < 0.01, respectively.
Arrest Characteristics
Of unshockable IHCAs, n=8/44 (18.2%) subsequently converted to a shockable rhythm later in the resuscitation, and conversely, n=3/19 (15.8%) of shockable IHCAs went on to become unshockable rhythms. Day and month of arrest are influential on survival and ROSC, respectively, however time of arrest was not significantly associated with either. See Figure 2 for outcomes per survival rhythm. Survivors had more arrests on their first day of admission, n=11/17 (64.7%), than non-survivors, n=13/46 (28.3%), p=0.02.
Length of Resuscitation
Resuscitation lasted less than 10 minutes in, n=37/63 (58.7%), of IHCA cases. In those that achieved ROSC, n=30/41 (73.2%), did so within 10 minutes. The median length of resuscitation lasted 5 minutes in survivors, which was significantly shorter than the median of 15 minutes, in patients who did not survive, p-value = 0.015.
Survivor Outcome
All survivors, (n=17), had a CPC score of one, post-arrest. One patient was subsequently lost to follow up. The remainder of survivors, (n=16/17), lived to at least 12 months post-arrest. There were three survivors who experienced a deterioration in their functional independence for activities of daily living.
Discussion
This is the first Irish report of in-hospital arrest data that has been contextualised by the manual review of patient notes. This approach was crucial, as nearly half of our initially defined study denominator subsequently did not satisfy the definition of an in-hospital cardiac arrest per the Utstein criteria 4, following this chart analysis. Our cardiac arrest incidence and survival rate was shown to be comparable to international standard9,10. Our survivors’ neurological outcomes approached 100%, and this correlated with excellent functional outcomes. Our cohort’s good outcome is somewhat unique in cardiac arrest literature, with a preservation of neurological function in less than 80% of cases11-13, typically. Survival at the ward level was lower than that seen in all other hospital locations (Table 2). The poorer outcomes seen in ward-based IHCA, seem related to prognostic favorability of a shockable rhythm, which we found to be less likely in a long-stay patient’s IHCA. We found that length of resuscitation was significantly shorter among survivors versus non-survivors, which is an established phenomenon4. Although our survival rate was excellent, the duration of our resuscitation attempts was shorter (in some cases) than some literature would advise15.
The issues of decreased observation, dilution of expertise, and de-escalated patient monitoring seen in ward care are a focus of the newly implemented NEWS system, as monitored and witnessed arrests are more likely to survive14. This new approach16 aims to identify physiologic deteriorations and allow early interventions. This has been shown to alter outcomes17. It is clear that IHCA context is different when occurring early versus later in a hospital admission. An acutely blocked coronary artery leading to an ischemic cardiac arrest is more likely to result in a shockable rhythm (a survival advantage)5, whereas a brewing septic milleu is more likely to lead to PEA or asystole14,18, with poor survival5. Recognition of change in clinical context could optimise survival. Since only the minority of cardiac arrests are survivable, prevention is a crucial goal, and it is hoped NEWS will facilitate an early recognition of disease progression, and prevention of deterioration toward cardiac arrest.
Not all Utstein variables were available for this study, due to documentation limitations. In the case of timing-based variables, such as time-to-defibrillation (in shockable rhythms)19, or time to arrival of cardiac arrest team20, values may be prognostic and can significantly influence outcome in IHCA. Length of resuscitation attempts were inconsistently reported. Sample size limited significance for some key Utstein variables. Our outcomes from IHCA are poorest on hospital wards when compared to other areas of the hospital. Those that survive have good functional and one year survival rates.
Correspondence: C Deasy
Department of Emergency Medicine, Cork University Hospital, Wilton, Cork,
Email: [email protected]
Acknowledgement
J O'Sullivan, for her large contribution to our data analysis.
References
1. Hunt EA, Mancini ME, Smyth M, Truitt TL, Investigators N (2009) Using the American Heart Association's National Registry of Cardiopulmonary Resuscitation for performance improvement. Joint Commission journal on quality and patient safety / Joint Commission Resources 35:13-20
2. Kouwenhoven WB (1961) Closed chest resuscitation of cardiac arrest. Chic Med 64:7-9
3. Bigham BL, Koprowicz K, Rea T, Dorian P, Aufderheide TP, Davis DP, Powell J, Morrison LJ, Investigators ROC (2011) Cardiac arrest survival did not increase in the Resuscitation Outcomes Consortium after implementation of the 2005 AHA CPR and ECC guidelines. Resuscitation 82:979-983.
4. Cummins RO, Chamberlain D, Hazinski MF, Nadkarni V, Kloeck W, Kramer E, Becker L, Robertson C, Koster R, Zaritsky A, Ornato JP, Callanan V, Allen M, Steen P, Connolly B, Sanders A, Idris A, Cobbe S (1997) Recommended guidelines for reviewing, reporting, and conducting research on in-hospital resuscitation: the in-hospital "Utstein style". American Heart Association. Annals of emergency medicine 29:650-679.
5. Peberdy MA, Kaye W, Ornato JP, Larkin GL, Nadkarni V, Mancini ME, Berg RA, Nichol G, Lane-Trultt T (2003) Cardiopulmonary resuscitation of adults in the hospital: a report of 14720 cardiac arrests from the National Registry of Cardiopulmonary Resuscitation. Resuscitation 58:297-308
6. National Cardiac Arrest Audit Homepage https://www.icnarc.org/CMS/ArticleDisplay.aspx?ID=acf00d90-5fdb-df11-8854-002264a1a658&root=RESEARCH&categoryID=b6fbea09-61db-df11-8854-002264a1a658.
7. Stiell IG, Nesbitt LP, Nichol G, Maloney J, Dreyer J, Beaudoin T, Blackburn J, Wells GA, Group OS (2009) Comparison of the Cerebral Performance Category score and the Health Utilities Index for survivors of cardiac arrest. Annals of emergency medicine 53:241-248.
8. Hazinski MF, Nolan JP, Billi JE, Bottiger BW, Bossaert L, de Caen AR, Deakin CD, Drajer S, Eigel B, Hickey RW, Jacobs I, Kleinman ME, Kloeck W, Koster RW, Lim SH, Mancini ME, Montgomery WH, Morley PT, Morrison LJ, Nadkarni VM, O'Connor RE, Okada K, Perlman JM, Sayre MR, Shuster M, Soar J, Sunde K, Travers AH, Wyllie J, Zideman D (2010) Part 1: Executive summary: 2010 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science With Treatment Recommendations. Circulation 122:S250-275.
9. Jones P, Miles J, Mitchell N (2011) Survival from in-hospital cardiac arrest in Auckland City Hospital. Emergency medicine Australasia : EMA 23:569-579.
10. Sandroni C, Nolan J, Cavallaro F, Antonelli M (2007) In-hospital cardiac arrest: incidence, prognosis and possible measures to improve survival. Intensive care medicine 33:237-245.
11. Sandroni C, Ferro G, Santangelo S, Tortora F, Mistura L, Cavallaro F, Caricato A, Antonelli M (2004) In-hospital cardiac arrest: survival depends mainly on the effectiveness of the emergency response. Resuscitation 62:291-297.
12. Peberdy MA, Ornato JP, Larkin GL, Braithwaite RS, Kashner TM, Carey SM, Meaney PA, Cen L, Nadkarni VM, Praestgaard AH, Berg RA (2008) Survival from in-hospital cardiac arrest during nights and weekends. JAMA : the journal of the American Medical Association 299 (7):785-792. doi:10.1001/jama.299.7.785
13. Danciu SC, Klein L, Hosseini MM, Ibrahim L, Coyle BW, Kehoe RF (2004) A predictive model for survival after in-hospital cardiopulmonary arrest. Resuscitation 62 (1):35-42. doi:10.1016/j.resuscitation.2004.01.035
14. Ballew KA, Philbrick JT, Caven DE, Schorling JB (1994) Predictors of survival following in-hospital cardiopulmonary resuscitation. A moving target. Archives of internal medicine 154 (21):2426-2432
15. Goldberger ZD, Chan PS, Berg RA, Kronick SL, Cooke CR, Lu M, Banerjee M, Hayward RA, Krumholz HM, Nallamothu BK (2012) Duration of resuscitation efforts and survival after in-hospital cardiac arrest: an observational study. Lancet 380 (9852):1473-1481.
16. McGinley A, Pearse RM (2012) A national early warning score for acutely ill patients. BMJ 345:e5310. doi:10.1136/bmj.e5310
17. Franklin C, Mathew J (1994) Developing strategies to prevent inhospital cardiac arrest: analyzing responses of physicians and nurses in the hours before the event. Critical care medicine 22 (2):244-247
18. Ebell MH (1992) Prearrest predictors of survival following in-hospital cardiopulmonary resuscitation: a meta-analysis. The Journal of family practice 34:551-558
19. Spearpoint KG, McLean CP, Zideman DA (2000) Early defibrillation and the chain of survival in 'in-hospital' adult cardiac arrest; minutes count. Resuscitation 44:165-169
20. Donnino MW, Salciccioli JD, Howell MD, Cocchi MN, Giberson B, Berg K, Gautam S, Callaway C (2014) Time to administration of epinephrine and outcome after in-hospital cardiac arrest with non-shockable rhythms: retrospective analysis of large in-hospital data registry. BMJ 348:g3028.
